Dear Editor,
Onychomatricoma (OM) is a rare benign neoplasm of nail matrix origin. The disease was first described by Baran and Kint in 1992 in a report of three cases.1 In some cases, it may present itself with important nail dystrophy, which makes its diagnosis a challenge. We report a rare case of OM in which we discussed the clinical and dermoscopic aspects of an exuberant lesion.
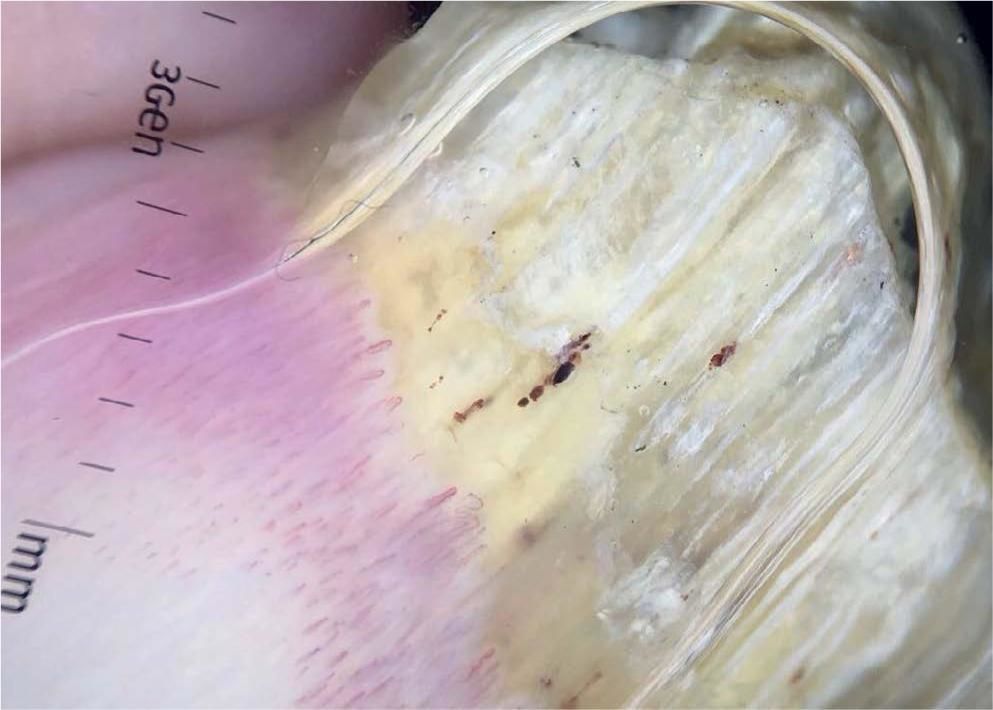
An 80-year-old male patient presented with an asymptomatic onychodystrophy on the left third toe beginning five years before. His pathological history revealed systemic arterial hypertension and dyslipidemia, without regular use of medications. On clinical examination we observed periungual erythema and a palpable hardened nodule on the proximal nail border, as well as xanthonychia and important onychodystrophy extending vertically from the nail bed in a filiform pattern (Figure 1). Onychoscopy of the nail plate revealed proximal splinter hemorrhages, white transverse lines, and yellowish areas (Figure 2). At the free edge of the nail, we observed dark cavitations in the middle of the subungual keratosis. After avulsion of the matrix and excision of the tumor, histopathological examination revealed epithelial proliferation in the nail matrix, sometimes papillomatous, and fibrous stroma, confirming the diagnosis of onychomatricoma (Figure 3).
Onychomatricoma is a rare, slow-growing neoplasm of the nail matrix – asymptomatic in most cases – that may rarely present with pain.2,3 It mainly affects Caucasian women around the age of 50. It is more common on the fingers than on the toes. However, this conclusion is questionable, since it is an asymptomatic lesion, and consequently, its alterations tend to be more noticeable when they occur on the fingers.2,3,4 Classically, it manifests itself with the formation of a nail plate of variable thickness, accentuation of the transverse curvature, splinter hemorrhages in the proximal portion, and cavitations in the plate that correspond to the projections arising from the matrix.1,2,4 It may also present itself as a nodule in the proximal nail fold or with hyperchromia. One of the clinical variants of OM is the giant or exuberant form, which is usually related to recurrent trauma and late diagnosis.2,4,5
Giant OMs are rarely reported in the literature. In 2016,4 Fierro-Arias et al. reported the case of a 53-year-old male patient with a one-year posttraumatic lesion on the right third toe, whose dermatological examination showed onychodystrophy, pachyonychia, and a yellowish-brown nail color. Prevezas et al., in 2016,5 also described an asymptomatic case of giant OM in a 73-year-old male patient with a lesion on the left first toe, with more than 10 years of evolution and a history of repeated local traumas. Examination revealed almost total dystrophy of the nail, pachyonychia, nail plate cavities, hemorrhagic spots, and yellowish color. As in the present case, both patients were men with toenail involvement and with similarities in the clinical findings. However, these cases were related to previous traumas, different from the patient described here. It is also worth noting the importance of dermoscopy in the diagnosis of this variant, since nail dystrophy distorts the morphological characteristics usually seen in the traditional clinical examination. Finally, all patients had a slow-growing lesion and delayed seeking a dermatologist.
OM diagnosis is based on clinical and histological examinations and may be complemented by imaging tests such as ultrasonography and nuclear magnetic resonance.2 Histology reveals a fibroepithelial neoplasm composed of a proximal and a distal zone. The proximal zone is characterized by invagination of the keratinized V-shaped epithelium; the distal zone is located in the region of the lunula and is characterized by digitiform projections that provoke perforations in the nail plate. The yellowish coloration seen at the clinical examination is caused by the thickening of the nail plate.2,4
The present case also had PAS positive septate hyphae on the histology of the excised lesion and clinical signs of onychomycosis in the nails of the other toes. It is known that there are several differential diagnoses of benign and malignant affections that affect the nail. Among them, onychomycosis is highlighted, since there is a discussion in the literature whether this is a predisposing factor for the development of OM or if OM is a predisposing factor for onychomycosis.2 In many cases, there is coexistence between the two conditions, as demonstrated in the literature by Kallis and Tosti in 2015.3
Finally, this report highlights important issues regarding an unusual giant clinical variant of onychomatricoma in concomitance with onychomycosis, and draws attention to dermoscopy as an ally for differential diagnosis.
Financial support: None.
Conflict of interests: None.